Introduction: The Quiet Risk Inside Senior Living
Over the past few years, I’ve visited senior living facilities, spoken with operators, and heard the same concerns repeated.
“Technology will reduce profits.”
“Caregivers will stop working if machines do the job.”
“We already struggle with staff performance, tech won’t fix that.”
These frustrations are real.
Caregivers are stretched. Margins are tight. Regulations are increasing.
But here’s the uncomfortable truth:
Ignoring AgeTech isn’t protecting margins, it’s increasing risk.
In 2026, facilities that fail to adopt the right technology aren’t just behind. They’re vulnerable – to safety failures, hospital readmissions, family dissatisfaction, and competitive displacement.
This article breaks down:
-
Why many facilities resist AgeTech
-
Why that thinking is flawed
-
What modern senior living leaders are doing differently
-
And how to implement technology without disrupting care
What Is AgeTech?
AgeTech refers to technology designed specifically to support aging populations. It includes:
-
Remote health monitoring
-
Fall detection systems
-
Smart sensors for mobility tracking
-
AI-powered predictive analytics
-
Telehealth platforms
-
Digital medication management
In simple terms:
AgeTech helps facilities detect risks early, respond faster, and improve outcomes — without replacing caregivers.
How Does AgeTech Work in Senior Living?
AgeTech systems typically function through:
-
Passive monitoring sensors (motion, bed, door, bathroom usage)
-
Wearables or pendants for fall detection
-
AI-driven analytics platforms
-
Real-time caregiver alerts
-
Family dashboards for transparency
Example Workflow:
-
A resident’s nighttime bathroom visits increase by 40%
-
System detects abnormal pattern
-
Care team receives alert
-
Nurse assesses for UTI risk
-
Early treatment prevents hospitalization
Without technology?
That pattern goes unnoticed – until symptoms worsen.
The Common Narrative From Facility Owners
Many operators express similar concerns:
1. “AgeTech Will Cut Into Profits”
They see:
-
Hardware costs
-
Monthly subscriptions
-
Training time
What they don’t calculate:
-
Cost of hospital readmissions
-
Liability from undetected falls
-
Staff turnover from burnout
-
Lost occupancy due to poor outcomes
2. “Caregivers Will Rely on Machines”
This fear assumes:
-
Technology replaces effort
-
Staff become disengaged
In reality:
Good technology removes low-value tasks and improves accountability.
3. “If Staff Don’t Perform Now, Tech Won’t Fix It”
True — but it can:
-
Provide data transparency
-
Create measurable workflows
-
Reduce ambiguity in care routines
People Focus on Costs – Not Care Outcomes
Many facilities treat AgeTech as a cost center.
But in healthcare, prevention always costs less than reaction.
Estimated Industry Data (Global Trends 2025–2026)
| Event | Average Cost |
|---|---|
| Fall with injury | $30,000+ per incident |
| Hospital readmission | $15,000–$25,000 |
| Staff replacement | 30–50% of annual salary |
| AgeTech monthly cost per resident | $50–$150 |
When viewed strategically, AgeTech becomes:
A risk management tool. Not an expense line item.
The Safety Gap No One Talks About
Residents in assisted living are high-risk for:
-
Infections
-
Dehydration
-
Wandering
-
Cognitive decline
-
Nighttime mobility issues
Without continuous monitoring:
-
Subtle changes go unnoticed
-
Symptoms are caught late
-
Emergency events increase
-
Liability rises
“We manage it when it happens” is not a strategy. It’s damage control.
Why AgeTech Matters More in 2026
1. Workforce Shortages Are Increasing
Global caregiver shortages are projected to worsen through 2030.
2. Resident Acuity Is Higher
Residents entering assisted living are older and medically complex.
3. Families Expect Transparency
Adult children expect:
-
Real-time updates
-
Digital communication
-
Data-backed safety
4. Governments Push Digital Health
Many regions now encourage remote monitoring to reduce hospital burden.
AgeTech is moving from optional innovation to operational standard.

Comparison: Traditional Monitoring vs AgeTech
| Feature | Traditional Model | AgeTech Model |
|---|---|---|
| Fall detection | Manual discovery | Instant alert |
| Night checks | Scheduled rounds | Behavior-triggered alerts |
| Documentation | Paper/manual | Automated data logs |
| Family updates | Reactive | Proactive dashboards |
| Risk detection | After symptoms | Before symptoms escalate |
AgeTech Does NOT Replace Caregivers – It Amplifies Them
What It Removes:
-
Constant manual checks
-
Guesswork
-
Documentation burden
What It Enables:
-
Focused intervention
-
Faster response
-
Data-driven care plans
-
Reduced burnout
Facilities that implement thoughtfully often report:
-
Higher staff satisfaction
-
Lower stress levels
-
Better prioritization
Technology handles monitoring. Humans handle compassion.
Real-World Example
A mid-sized assisted living facility implemented:
-
Passive fall detection
-
Bed exit alerts
-
AI mobility trend tracking
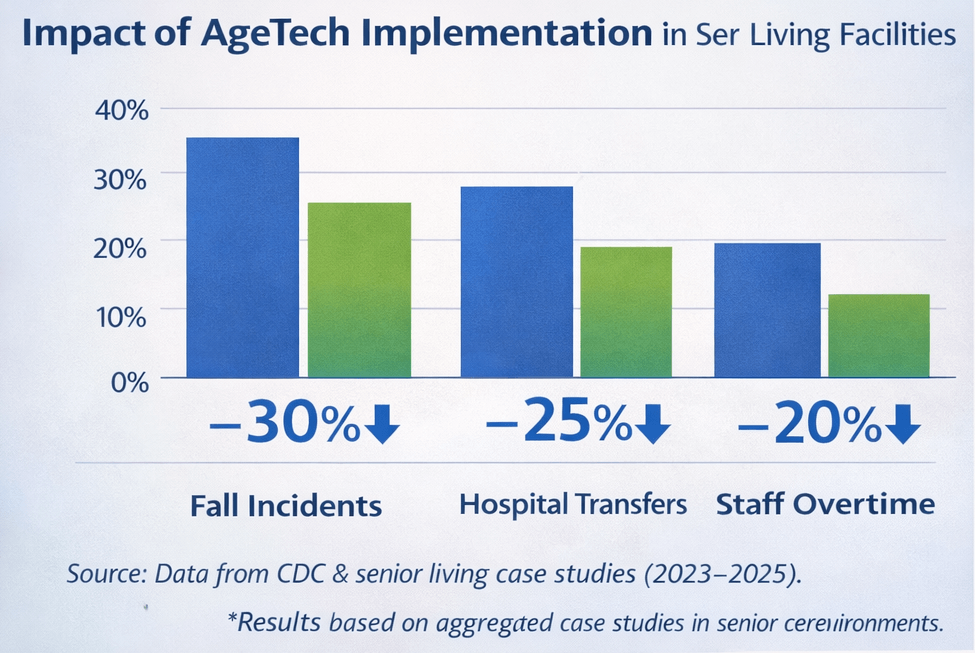
Within 12 months:
-
28% reduction in fall-related hospital transfers
-
19% reduction in nighttime staff overtime
-
Increased family satisfaction scores
The investment paid for itself within one year.
Step-by-Step Framework: How to Implement AgeTech Correctly
Step 1: Define Your Risk Areas
-
Falls?
-
Night wandering?
-
Medication adherence?
-
Hospital readmissions?
Step 2: Start Small
Pilot with:
-
One wing
-
High-risk residents
-
Specific use case (e.g., fall detection)
Step 3: Train Staff With Purpose
Explain:
-
This is support, not surveillance
-
Alerts improve efficiency
-
Documentation becomes easier
Step 4: Measure ROI
Track:
-
Incident rates
-
Response times
-
Staff overtime
-
Hospital transfers
-
Family satisfaction
Step 5: Scale Strategically
Expand based on measurable impact.
Common Mistakes Facilities Make
-
Buying technology without workflow planning
-
Failing to train staff properly
-
Choosing cheapest vendor over proven solution
-
Not communicating benefits to families
-
Treating it as an IT project instead of care strategy
Pro Tips From Industry Leaders
-
Choose passive systems over wearable-dependent solutions
-
Prioritize integration with existing EHR systems
-
Involve caregivers in vendor selection
-
Use data for marketing differentiation
-
Highlight safety improvements in occupancy tours
Tools & Resources to Explore
-
Remote monitoring platforms
-
AI mobility analytics tools
-
Fall detection sensor providers
-
Telehealth integration platforms
-
Staff workflow automation software
FAQs
1. Why are senior living facilities slow to adopt AgeTech?
Many facilities hesitate due to cost concerns, fear of disrupting workflows, and misconceptions that technology replaces caregivers. However, most resistance stems from short-term budget thinking rather than long-term risk management strategy.
2. What are the biggest risks of not using AgeTech in assisted living?
The biggest risks include undetected falls, delayed emergency response, higher hospital readmissions, increased liability exposure, staff burnout, and declining occupancy due to family concerns about safety transparency.
3. How does AgeTech improve caregiver efficiency?
AgeTech reduces manual checks and paperwork by sending alerts only when intervention is needed. This helps caregivers prioritize high-risk residents and spend more time on meaningful interaction instead of routine monitoring.
4. Can small senior living facilities afford AgeTech?
Yes. Many modern solutions are subscription-based and scalable. Facilities can start with high-risk residents or specific use cases like fall detection and expand gradually based on measurable ROI.
5. Does AgeTech increase liability risks?
No. When implemented properly, AgeTech often reduces liability by documenting incidents, providing timestamped alerts, and demonstrating proactive safety measures to regulators and families.
6. What types of AgeTech are most effective in 2026?
The most effective solutions include passive fall detection sensors, AI mobility analytics, remote patient monitoring systems, telehealth integration platforms, and automated care documentation tools.
7. How long does it take to see ROI from AgeTech?
Many facilities report measurable ROI within 6–12 months due to reduced hospital transfers, lower overtime costs, improved occupancy rates, and decreased insurance claims.
8. How do families respond to tech-enabled senior living communities?
Families generally respond positively. Transparency dashboards, real-time alerts, and digital communication tools increase trust, reduce anxiety, and strengthen long-term retention.
Key Takeaways
-
Ignoring AgeTech increases operational risk.
-
Technology enhances – not replaces – human care.
-
Early detection reduces hospitalizations and costs.
-
Families increasingly expect digital transparency.
-
2026 demands data-driven senior living operations.
Related Topics
About the Author
Widelly
widelly-admin · 13 articles published
Expert contributor at Widelly, sharing insights on B2B and B2C growth strategies.
